Age Related Macular Degeneration (AMD)
Age-Related Macular Degeneration (AMD) is the leading cause of vision loss in older American adults. AMD is also the most common diagnosis for a patient to be referred to Louisiana Retina Center. AMD is an age related condition that causes deterioration of the central vision. Patients with AMD may note a worsening of their central vision while retaining good peripheral vision. There are two types, Dry AMD and Wet AMD. Dry AMD comes first and may later progress to Wet AMD. Wet is typically causes the most severe vision loss.
The macula is the central part of the retina responsible for central vision and detailed visual tasks. Many patients with macular degeneration share a common misconception that the disease will automatically progress to blindness. It will only effect the central vision, leaving the peripheral or side vision intact.
In macular degeneration, patients suffer varying degrees of destruction to this tissue and can experience a wide spectrum of visual problems. These include, but are not limited to:
- Blurred central vision
- Increasing difficulty with reading
- Patchy visual loss
- Distortion or warping of straight objects
However, even patients with advanced macular disease tend to retain excellent peripheral vision.
WHO IS AT RISK?
Macular degeneration primarily affects people over fifty years of age and becomes more common with each additional decade.
Additionally, a number of risk factors predispose certain people to the development and progression of the disease, including:
- Cigarette smoking
- Poor nutrition
- Cardiovascular disease
- Having a family member with AMD
Regarding the last risk factor, much research has been done regarding the genetics of macular degeneration. Although there is currently no way to definitively predict who will or will not develop AMD, those with affected relatives are at significantly higher risk. As a result, adult relatives of AMD patients should schedule an appointment with a retina specialist and undergo a baseline evaluation and dilated exam.
WHAT TESTS ARE HELPFUL IN AIDING DIAGNOSIS?
Dry and wet macular degeneration impact vision in different ways and are also treated quite differently. Dr. Blem will use a variety of clinical tests and exam techniques to better characterize your individual situation, make an accurate diagnosis, and optimize treatment.
During an initial visit for macular degeneration, patients typically undergo two tests: Fluorescein Angiography (FA) and Optical Coherence Tomography (OCT).
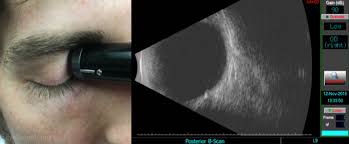
FA is considered the “gold standard” for differentiating between dry and wet AMD. It involves the injection of a small amount of sodium based dye through a patient’s peripheral vein – usually the arm or hand. Shortly after, a certified ophthalmic angiographer will take a series of time-dependent retinal photographs. The injected dye lights up the retina’s intricate vascular network. This helps our specialists pinpoint areas of leakage in those patients with wet macular degeneration and target specific zones with specialized laser therapy when needed.
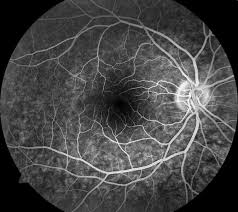
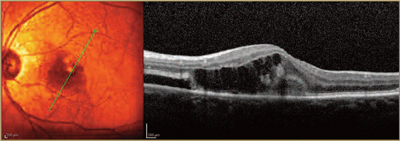
OCT is a newer, non-invasive, quick exam that has gained universal acceptance during the last decade and is now used by many ophthalmologists to visualize the retinal microarchitecture. Using reflected light rays, OCT provides a detailed, highly magnified, cross-section view of a patient’s macula. Sometimes, it will uncover tiny areas of fluid or retinal irregularity not readily apparent to a retina specialist during a microscopic exam.
Normal OCT
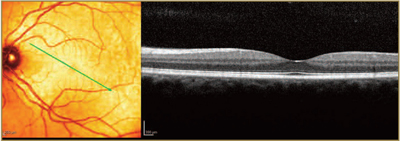
Dry AMD OCT
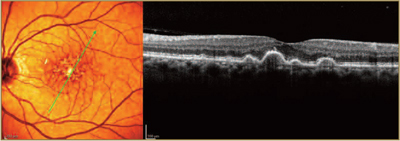
Wet AMD OCT
PATIENTS PLAY AN IMPORTANT ROLE IN DIAGNOSIS AND CARE
Despite recent advances in ophthalmic imaging, there is no single test that can be relied upon to direct treatment and clinical decision-making. A patient’s relationship Dr. Blem is at the core of our practice philosophy, and good patient-physician communication is critical. Important decisions about retinal health are very much a joint effort. The patient’s perception of his or her visual health and the patient’s perception of any vision changes, however slight, is every bit as important in directing care as are the clinical tests.
As a result, every patient diagnosed with macular degeneration should establish a daily routine for monitoring their own vision. This is most simply and reliably performed with an Amsler grid, a simple graph paper-like patchwork of straight vertical and horizontal lines. We have a copy of one including directions on how to use it on our website under patient instructions.
Printable Amsler Grid
Amsler Grid
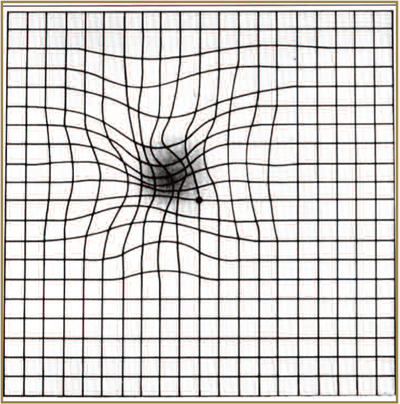
Amsler Grid as it might appear to someone with age-realated macular degeneration.
Often, patients with subtle progression of macular disease will report new “waviness” or “missing areas” when monitoring their grid. Should you or a family member notice new changes on an Amsler grid, contact us promptly. One of our trained ophthalmic nurses is always available to consult with you by phone. As a general rule, patients who receive treatment in a more timely fashion tend to fare better than those who delay evaluation by a retina specialist.
WHAT TREATMENTS ARE AVAILABLE?
Dry AMD
Dry macular degeneration is treated by targeting the risk factors. Stopping smoking is the single most important controllable risk factor for macular degeneration. Dr. Blem will help with a stop smoking program for you should you so wish.
Improving nutrition with multivitamins has been shown in multiple studies to help prevent or slow the progression of Dry AMD. Dr. Blem and his staff will discuss these vitamins and your options with you.
Wet AMD
Medical researchers have thrown themselves fully into the battle against macular degeneration, and dramatic progress has been made in the effort to combat age-related vision loss. The most promising new treatments are medications that block a molecule called VEGF (Vascular Endothelial Growth Factor). VEGF causes growth of “leaky” blood vessels in wet macular degeneration. These medications include Avastin, Lucentis, and Eylea. All of these medications are introduced directly into the eye through a tiny needle. While the thought of an “eye shot” might cause many to cringe, in our experience, there is little, if any, patient discomfort, and the spectacular visual gains far outweigh any fears.
In contrast to prior therapies, these medications have actually improved vision for many patients with wet macular degeneration. Several large national and international studies have shown that Avastin, Lucentis, and Eylea all work well. Dr. Blem and his team will discuss with you which medication may be best suited for your situation.
In general, repeated injections are the norm in order to keep Wet AMD from recurring.

